

Authors: Akash Virupakshaiah, MD; Sonika Agarwal, MBBS, MD
Children’s Hospital of Philadelphia , Perelman School of Medicine at the University of Pennsylvania
Reviewed: June 2021
JUMP TO
Disorder Overview
SUMMARY
Hypoxic ischemic encephalopathy (HIE) is a type of brain disorder or dysfunction that occurs early in life. It is due to a combination of:
- Hypoxia: when brain does not receive enough oxygen for a period of time
- Ischemia: when blood flow to the brain is restricted for a period of time
- Encephalopathy: a brain disorder or dysfunction of the brain
HIE is one type of neonatal encephalopathy (NE). NE is a broad term referring to several brain-related conditions in newborns. NE conditions cause problems in babies’ central nervous systems. The problems begin within the first several days after birth. HIE can happen before birth (during pregnancy), at birth, or immediately after birth. HIE is a relatively rare event, occurring in 2 to 4 of every 1,000 births.
Symptoms and outcomes vary. They depend on the cause and severity of the HIE. Some children experience no health issues. Some have mild to moderate effects. Still others have more severe effects. Severe HIE can cause permanent disability and affect development. It can lead to developmental delay. It can also lead to cerebral palsy, seizures, epilepsy and/or cognitive impairment.
Like the brain, other organs are also dependent on blood supply and oxygen. A reduced blood or oxygen supply can affect these organs, too. For instance, the heart, liver, kidneys, and bowels may be affected alongside the brain. These organs may not function normally. Sometimes, affected organs can recover complete function. However, if the brain sustains injury, it may lead to long-term neurodevelopmental deficits. The duration and severity of the hypoxia and ischemia matter. They determine the severity of any deficits in development and otherwise.


CAUSES
HIE can occur during:
- Fetal development (in the prenatal period, or pregnancy)
- Labor and delivery
- Following birth (in the postnatal period)
Fetal Development
The risk factors and causes of HIE during fetal development include:
- Problems associated with blood flow to the placenta
- Congenital or in-utero infections such as (toxoplasma, CMV etc. can predispose to brain injury)
- Maternal drug or alcohol abuse
- Severe fetal anemia
- Fetal heart disease
- Fetal lung malformations
- Preeclampsia
- Maternal diabetes with vascular disease
- Other medical disorders in pregnancy can limit blood flow to the placenta
Labor and Delivery
The risk factors and causes of HIE during labor and delivery include:
- Placental abruption
- Placenta previa
- Uterine rupture
- Problems with the umbilical cord, such as cord prolapse and knots (lead to drop in fetal heart and HIE)
- Bleeding from the placenta
- Prolonged labor
- Slow fetal heart rate due to labor complications
- Maternal infections – chorioamnionitis
Following Birth
The risk factors and causes of HIE following birth:
- Prematurity
- Birthing trauma to the brain or skull
- Traumatic delivery
- Lung or heart disease
- Infections (sepsis, other)
- Maternal or placental complications leading to low blood pressure in the baby during delivery
- Respiratory failure
- Cardiac arrest
SIGNS AND SYMPTOMS
Symptoms of HIE vary. They depend primarily on the severity of the underlying brain damage. The symptoms can be divided into three types: mild, moderate, and severe.
Mild HIE
Symptoms of mild HIE often resolve within a few weeks. They include:
- Irritability
- Excessive crying or sleeping
- Feeding problems
- Abnormal deep tendon reflexes
- High or stiff muscle tone (hypertonia)
Moderate HIE
Symptoms of moderate HIE include:
- Poor grasp
- Inadequate sucking response
- Low muscle tone (hypotonia), floppiness, or no reflexes
- Episodes of apnea, or stopped breathing
- Seizures in the newborn
Severe HIE
Symptoms of severe HIE include:
- Lack of response to external stimulus
- Severe seizures that cannot be helped with medication
- Irregular or abnormal breathing
- Extreme floppiness (hypotonia)
- Abnormal posturing or body positioning
- Abnormal eye movements
- Abnormal heart rate and blood pressure
- Cardiorespiratory failure
- Other associated organ-injury-related symptoms involving the kidney, liver, and multisystem failure


PREVENTION
HIE can sometimes be prevented by appropriately managing maternal risk factors and early diagnosis and management of pregnancy related complications.
First, risk factors can be reduced with care throughout pregnancy. Regular visits with a health care provider are essential.
These prenatal visits can:
- Help with management of medical complications during pregnancy
- Help with immunizing mother
- Prevent low birth weight
- Prevent premature birth
- Proper nutrition and vitamin supplements
Second, avoiding maternal bodily injuries is important.
For instance, it helps to:
- Wear a seat belt
- Use a bike or motorcycle helmet
- Avoid risky exercises and behaviors
Third, alcohol, tobacco, and illegal drugs have been linked to HIE. Avoiding them can lower the risk of HIE.
DIAGNOSIS
HIE is suspected based on:
- Known risk factors
- Pregnancy and labor/birth history
- Medical records from birth documenting fetal:
- Heart rate
- Activity
- Color
- Movements
- Breathing
- Requirements for support and resuscitation around time of birth
To diagnose HIE, a complete physical exam is performed. The medical team examines the baby for symptoms and signs of HIE. Additional labs may help aid the diagnosis. For instance, cord blood tests can help.
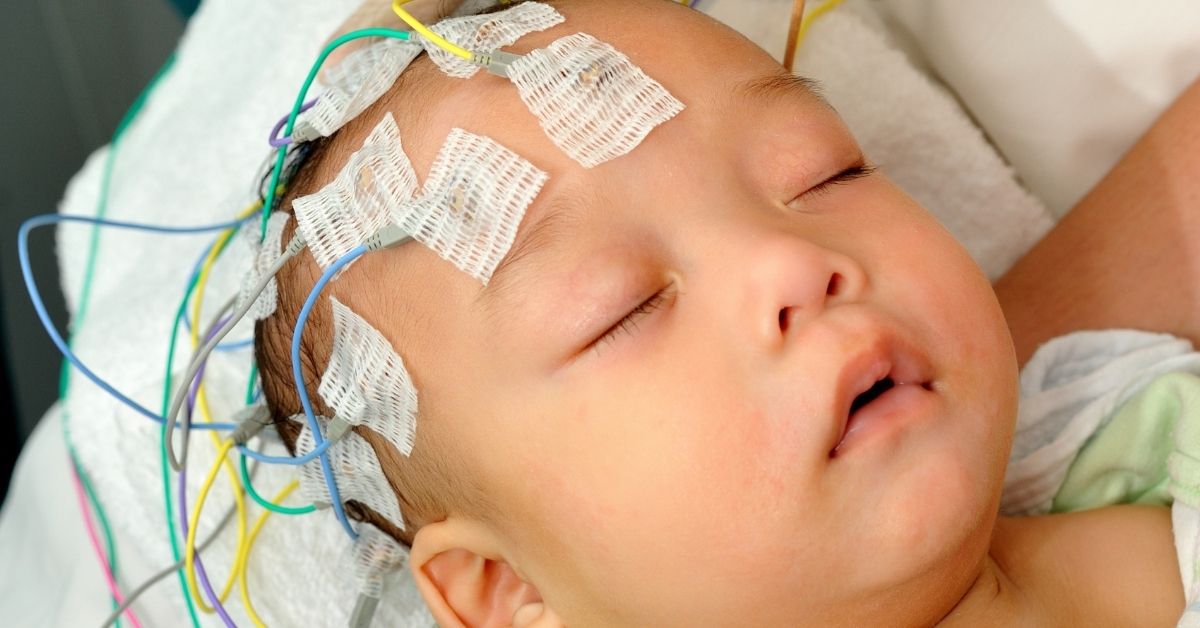
Once a diagnosis is suspected, a baby is usually monitored for signs of brain dysfunction. For instance, they may be checked for seizure activity. This is done using an electroencephalogram (EEG). An EEG measures the electrical activity of the brain. Then, continuous video monitoring is used as available. Video helps because signs of seizures may be very subtle and not noticeable in babies.
Magnetic resonance imaging (MRI) is also used. MRI can take pictures of the brain. It can look for signs of brain injury. It can also look for other causes for encephalopathy, such as:
- Stroke
- Hemorrhage (bleeding)
- Brain malformations.

TREATMENT AND THERAPIES
Treatment begins as soon as a diagnosis of HIE is made. This starts in the neonatal intensive care unit (NICU).
Here is what to expect in the NICU:
Brain Cooling
Also known as therapeutic hypothermia.
Therapeutic cooling is the standard of care for HIE. Much research suggests that the extent of brain injury can be reduced when the brain is cooled. It needs to be cooled a few degrees below normal body temperature.
During cooling, the baby is placed on a cooling blanket. The baby’s temperature is closely monitored. The cooling period lasts for three days.
Then the baby is gradually re-warmed to normal temperature.
EEG
Video monitoring
Blood tests
Imaging studies and discussion
When the cooling period is done, the baby will undergo additional imaging studies. Imaging studies take pictures of the brain.
MRI is an important tool that can help assess the extent of brain injury. A pediatric neurologist usually reviews results of MRI, the EEG, and over all clinical course with the family. They will discuss prognosis for the neurodevelopmental outcome.
They will also help plan for long–term follow up care, early intervention, and other supports.
Therapy

Here is what to expect after discharge from the NICU:
Progress checks
OUTLOOK
Outcomes vary depending on the severity of HIE. Some babies do well. They may not have long-lasting effects. Others may require extensive support. They may be intellectually disabled.
Some long-term complications can result from HIE.
They include:
- Developmental delay
- Cerebral palsy
- Intellectual disability
- Seizures
- Hearing and vision problems
- Feeding issues
- Mental health concerns
- Contracture, a tightening of the muscles or other tissues
- Spinal deformities
- Sensory issues


Resources
ORGANIZATIONS/GROUPS
Hope for HIE
The mission of Hope for HIE is to improve the quality of life for children and families impacted by Hypoxic Ischemic Encephalopathy through awareness, education, and support.
Hope for HIE hosts a private Facebook group with over 6,000 members.


PUBLICATIONS
JCN: What Your Pediatric Neurologist Wants You to Know: Neonatal Neurology
Podcast from SAGE Neuroscience and Neurology/Journal of Child Neurology (JCN). JCN’s Residents and Fellows Board Director, Dr. Alison Christy, interviews Dr. Sonika Agarwal, a neonatal neurologist from Children’s Hospital in Philadelphia.
Child Neurology Foundation (CNF) solicits resources from the community to be included on this webpage through an application process. CNF reserves the right to remove entities at any time if information is deemed inappropriate or inconsistent with the mission, vision, and values of CNF.
Research
ClincalTrials.gov for Neonatal Hypoxic Ischemic Encephalopathy and Neonatal Encephalopathy are clinical trials that are recruiting or will be recruiting. Updates are made daily, so you are encouraged to check back frequently.
ClinicalTrials.gov is a database of privately and publicly funded clinical studies conducted around the world. This is a resource provided by the U.S. National Library of Medicine (NLM), which is an institute within the National Institutes of Health (NIH). Listing a study does not mean it has been evaluated by the U.S. Federal Government. Please read the NLM disclaimer for details.
Before participating in a study, you are encouraged to talk to your health care provider and learn about the risks and potential benefits.
Family Stories
Hope for HIE shares hundreds of Family Stories, giving hope and inspiration to those living with Hypoxic Ischemic Encephalopathy.
The information in the CNF Child Neurology Disorder Directory is not intended to provide diagnosis, treatment, or medical advice and should not be considered a substitute for advice from a healthcare professional. Content provided is for informational purposes only. CNF is not responsible for actions taken based on the information included on this webpage. Please consult with a physician or other healthcare professional regarding any medical or health related diagnosis or treatment options.
References
Douglas-Escobar M, Weiss MD. Hypoxic-ischemic encephalopathy: a review for the clinician. JAMA Pediatr. 2015 Apr;169(4):397-403. doi: 10.1001/jamapediatrics.2014.3269.PMID: 25685948 Review.
Yıldız EP, Ekici B, Tatlı B. Neonatal hypoxic ischemic encephalopathy: An update on disease pathogenesis and treatment. Expert Rev Neurother. 2017 May;17(5):449-459. PMID: 27830959; https://doi.org/10.1080/14737175.2017.1259567
C. Weeke, MD, PhD, Floris Groenendaal, MD, PhD , Kalyani Mudigonda, MD , Mats Blennow, MD, PhD , Maarten H. Lequin, MD, PhD , Linda C. Meiners, MD, PhD, Ingrid C. van Haastert, MA, PhD , Manon J. Benders, MD, PhD, Boubou Hallberg, MD, PhD, , and Linda S. de Vries, MD, PhD. A Novel Magnetic Resonance Imaging Score Predicts Neurodevelopmental Outcome After Perinatal Asphyxia and Therapeutic Hypothermia Lauren. J Pediatr 2018;192:33-40.
Thank you to our 2023 Disorder Directory partners:





