

Authors: Margaret Means, MD; Sonika Agarwal, MBBS, MD, Children’s Hospital of Philadelphia
Reviewed: August 2021
SUMMARY
Megalencephaly is a condition in which a child’s brain is abnormally large. In this condition, the weight of the brain is greater than average for the age and sex of the child. It may also be called macrencephaly.
The condition may have different genetic or metabolic causes. A diagnosis is made by:
- Measuring the head
- Looking at images of the brain
Children usually have developmental delays. They may have seizures or other neurological issues, too. Treatment usually includes several kinds of therapy. These therapies can help with delays. They can help with other symptoms, too.
JUMP TO
Disorder Overview
DESCRIPTION
Children with megalencephaly have a brain that is larger than average. This is determined with a comparison to other children of the same age and sex.
Various conditions can cause an increase in the number or size of brain cells. This may result in a larger brain. Because of the large brain, children with megalencephaly also have a large head.
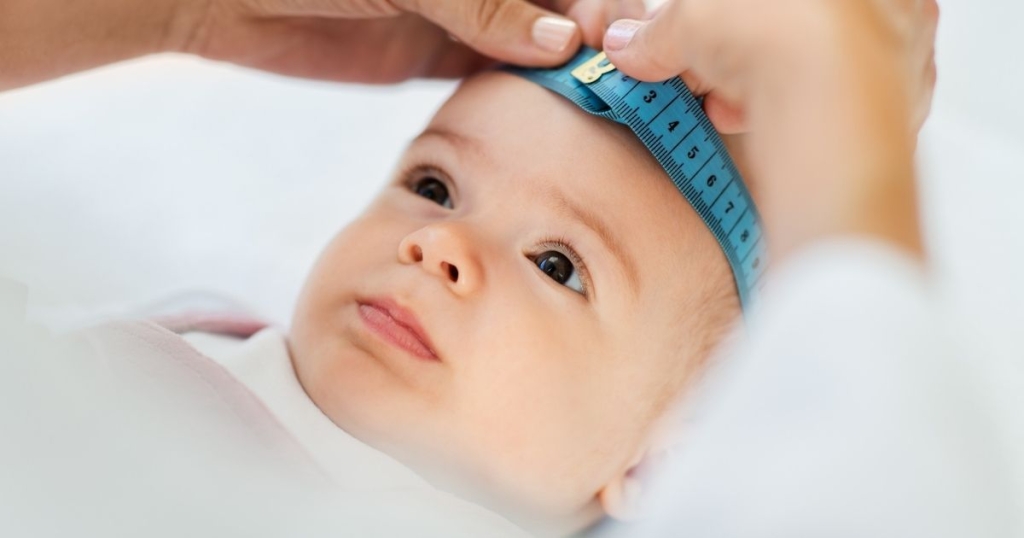

Head circumference is the total distance around the head. It is usually measured with a tape measure at physical exams. In megalencephaly, a child’s head size is above the 97th percentile. In other words, it measures larger than 97% or more of other children’s heads. This comparison is made with standard size charts. The standards are provided by organizations like the CDC. Comparisons may also be made to parents’ or siblings’ head sizes.
Megalencephaly affects more males than females.
Macrocephaly Vs. Megalencephaly
It is important to differentiate between macrocephaly and megalencephaly.
Macrocephaly refers to an increased head circumference. It may have various causes. They can include:
- Abnormalities of the skull’s bone structures
- An increase of fluid collection in the brain or surrounding the brain
- An enlargement of the brain (megalencephaly)
Having macrocephaly does not necessarily mean a child has a brain abnormality. It only indicates a large head. The brain may be normal. Some families have a tendency for larger head size in children and adults, who may be otherwise normal neurologically or have no other symptoms.
Megalencephaly refers to an increased brain size. It reflects the growth of abnormal brain structures. This can happen at various steps of brain development. Megalencephaly is more severe than macrocephaly. It is more likely to include:
- Developmental delays
- Learning delays
- Seizures
- Other neurologic symptoms
Not all people with a larger head have an enlarged brain. However, most people with an enlarged brain do have a larger head, too.
SIGNS AND SYMPTOMS
Signs
The primary sign of this condition is a large head. The head may be large at birth. Or it may become larger as a child grows.
Measuring the head:
- Ultrasound. This may be used before birth or after birth.
- Tape measure. This may be used after birth or at childhood doctor’s visits.

Symptoms
This condition may look different in different cases:
- Large head only. Sometimes, a large head is the only symptom.
- Developmental delays. Most children with this condition have delays. Intellectual disabilities may appear as they grow older.
- Other organs affected. This condition may be part of an underlying genetic syndrome. The underlying syndrome can affect organ systems besides the brain.
In addition to the above, children with this condition may have:
- Seizures
- Movement issues
- Balance issues
- High muscle tone
- Low muscle tone
- Feeding issues
- Breathing issues
- Dark- or light-colored spots on the skin
- Vision problems
CAUSES
Most causes of this condition are genetic. Genetic causes can occur for different reasons. They may be:
- Inherited from parents
- Due to a new change in a child’s gene

Specific genetic causes for this condition include:
Neurocutaneous disorders
Metabolic disorders
Metabolic disorders may be inherited or due to new mutations. They cause problems with how chemical reactions happen in the body. They can affect how the body produces energy. These disorders may lead to a buildup of toxins in brain cells. This can make brain cells larger than normal. Then, brain cells may not function properly. Abnormal brain development is sometimes the result.
DIAGNOSIS AND LABORATORY INVESTIGATIONS
Clinical Exams
A diagnosis may involve measuring a child’s head. Doctors can measure the circumference, or distance around, a child’s head after birth.
A child with suspected macrocephaly or megalencephaly will be referred to a child neurologist. The neurologist will:
- Take a complete health history
- Perform a physical exam
- Recommend any further testing needed
Referral to other specialists may also be needed. This will depend on the symptoms and the other organs involved. Specialists may include:
- Geneticists. They can help with genetic testing.
- Endocrinologists. They focus on hormones and the metabolic functions of the body.
- Ophthalmologists. These are eye doctors. They can perform eye exams.
- Dermatologists. These are skin doctors. They can perform skin exams.
Brain Imaging
Pictures taken of the brain can provide information to doctors. The pictures can show differences in how a child’s brain developed. Two types of imaging are most common:
- Ultrasound. Used prior to or after birth.
- Magnetic resonance imaging (MRI). Used prior to, or after, birth.
In recent years, when abnormalities are seen on pregnancy ultrasound, a woman may receive an MRI as well. An MRI can offer a better idea of the head size of an unborn baby. This helps doctors and parents know if there may be brain abnormalities even before a baby is born. Such infants will be closely followed by specialists in children’s brain disorders.
Genetic Tests
Genetic tests on a child may reveal likely causes of a case of megalencephaly. The child’s parents may then also be tested. Testing parents can show whether a genetic mutation is inherited or new in the patient. It can help determine how likely it is that the condition will appear again in future pregnancies. A genetic counselor can help interpret test results.
Genetic tests may include:
- A chromosomal microarray. This tests whether there are missing or extra chromosomes or chromosome pieces.
- A megalencephaly panel. This is a test that focuses only on genes commonly associated with the condition.
- Whole exome sequencing. This tests some of the most important sections (exome) of a person’s whole genome. However, it may miss important findings because it has such a large scope and we are unable to test all possible genes with this test.
Blood Tests
TREATMENT AND THERAPIES
Treatment usually focuses on symptoms. If the case of megalencephaly is severe, a child may need long-term treatment.
Therapy
Seizure Treatment
Some patients with this condition have seizures. In these cases, antiseizure medicine may be needed.
There are multiple antiseizure medicines available, like oxcarbazepine, levetiracetam, topiramate, zonisamide, lacosamide, clobazam, etc. However, sometimes, no medicine can control the seizures. In these cases, alternatives may be considered. Alternatives include:
- Special diets: ketogenic diet
- Surgery
OUTLOOK
Prognosis varies greatly. It depends on:
- The severity of the condition
- The underlying cause of the condition
Severe Cases
In severe cases:
- Lifespan may be shortened. Lifespan may be shortened due to seizures, feeding or swallowing issues, or other problems. Some causes of megalencephaly, particularly metabolic causes, can lead to a shorter lifespan due to progressive brain dysfunction.
- Disability may be significant. Significant intellectual disability is common in this condition. Children may need help with everyday tasks as they grow up.
- Education may be more challenging. Children may need help in school. They may need special education support or therapy.
Milder Cases
In milder cases:
- Lifespan may be normal. Lifespan may be normal.
- Disability may be milder. Children may have only mild delays. They may be able to perform everyday tasks independently.
- Education may be less challenging. Children may only need a small amount of help in school.


RELATED DISORDERS
Disorders related or similar to this condition include:
- Hemimegalencephaly. This is a rare condition in which only one side of the brain in enlarged. It is also called unilateral megalencephaly.
- Macrocephaly. This describes a large head, specifically one larger than 97% or more of other children of the same age and sex. Having macrocephaly does not necessarily mean a child has a brain abnormality. It only indicates a large head. The brain may be normal. Some families have a tendency for larger head size in children and adults, who may be otherwise normal neurologically or have no other symptoms as described above.
- Various genetic disorders. There are many different genetic disorders now known to cause megalencephaly. More of them will likely be discovered over time.
Resources
Organizations
Pediatric Epilepsy Surgery Alliance
The Pediatric Epilepsy Surgery Alliance (formerly known as The Brain Recovery Project) enhances the lives of children who need neurosurgery to treat medication-resistant epilepsy. They empower families with research, support services, and impactful programs before, during, and after surgery. PESA’s programs include research-based, reliable information to help parents and caregivers understand when a child’s seizures are drug-resistant; the risks and dangers of seizures; the pros and cons of the various neurosurgeries to treat epilepsy; the medical, cognitive, and behavioral challenges a child may have throughout life; school, financial aid, and life care issues. PESA’s resources include a comprehensive website with downloadable guides, pre-recorded webinars, and virtual workshops; an informative YouTube channel with comprehensive information about epilepsy surgery and its effects; a private Facebook group (Education After Pediatric Epilepsy Surgery) with over 300 members; Power Hour (bi-monthly open forums and live virtual workshops on various topics); and free school training to help your child’s education team understand the impact of their epilepsy surgery in school. Their Peer Support Program will connect you with a parent who has been there. The Pediatric Epilepsy Surgery Alliance also hosts biennial family conferences and regional events that allow families to learn from experts, connect with other families, and form lifelong friendships. They also provide a travel scholarship of up to $1,000 to families in need to fund travel to a level 4 epilepsy center for a surgical evaluation.
In addition, PESA has resources for medical professionals to assist in helping clinicians help the parents of their patients find the resources they need after surgery. Educators and therapists will also find helpful resources and information, including videos, guides, and relevant research. Patients who have undergone surgery are encouraged to register with the Global Pediatric Epilepsy Surgery Registry to help set future research priorities.
Child Neurology Foundation (CNF) solicits resources from the community to be included on this webpage through an application process. CNF reserves the right to remove entities at any time if information is deemed inappropriate or inconsistent with the mission, vision, and values of CNF.
Research
ClinicalTrials.gov for Megalencephaly (birth to 17 years)
These are clinical trials that are recruiting or will be recruiting. Updates are made daily, so you are encouraged to check back frequently.
ClinicalTrials.gov is a database of privately and publicly funded clinical studies conducted around the world. This is a resource provided by the U.S. National Library of Medicine (NLM), which is an institute within the National Institutes of Health (NIH). Listing a study does not mean it has been evaluated by the U.S. Federal Government. Please read the NLM disclaimer for details.
Before participating in a study, you are encouraged to talk to your health care provider and learn about the risks and potential benefits.
The information in the CNF Child Neurology Disorder Directory is not intended to provide diagnosis, treatment, or medical advice and should not be considered a substitute for advice from a healthcare professional. Content provided is for informational purposes only. CNF is not responsible for actions taken based on the information included on this webpage. Please consult with a physician or other healthcare professional regarding any medical or health related diagnosis or treatment options.
References
Megalencephaly Information Page. National Institute of Neurological Disorders and Stroke. Published March 27, 2019. https://www.ninds.nih.gov/Disorders/All-Disorders/Megalencephaly-Information-Page
Megalencephaly. The Cleveland Clinic. Published June 30, 2015. https://my.clevelandclinic.org/health/articles/6069-megalencephaly
Swaiman KF. Swaiman’s Pediatric Neurology: Principles and Practice. Edinburgh: Elsevier; 2018. Ch 28: Disorders of Brain Size. p. 208-217. https://www.worldcat.org/title/swaimans-pediatric-neurology-principles-and-practice/oclc/993643240
Pina-Garza JE. Fenichel’s Clinical Pediatric Neurology. London: Elsevier Saunders; 2013. Ch 18: Disorders of Cranial Volume and Shape. p. 356-358. https://www.worldcat.org/title/fenichels-clinical-pediatric-neurology/oclc/1036254009
Thank you to our 2023 Disorder Directory partners:





