
Author: Shaun A. Hussain, MD
UCLA Mattel Children’s Hospital
Reviewed: July 2021
SUMMARY
Infantile spasms is a kind of epilepsy. It usually begins in children who are less than one year old.
Other names for infantile spasms include:
- West syndrome
- Epileptic spasms
- Infantile spasms syndrome
Children with infantile spasms typically have clusters of short seizures. They often exhibit developmental problems.
A diagnosis of infantile spasms can be made by looking at a child’s movements and performing an electroencephalogram (EEG) to evaluate their brainwaves. Diagnosing and treating infantile spasms is an urgent matter. If not treated, the disorder can permanently harm development. The main treatments include hormonal therapy and vigabatrin, an anti-seizure medicine.
Infantile spasms may occur in children without prior medical problems. However, most children get infantile spasms after the diagnosis of another brain disorder. The long-term outcome for children with infantile spasms varies a lot. It depends on the cause of the disorder. Some children with rapid diagnosis and successful treatment will have a normal health outcome. However, many children will have poor outcomes.
Poor outcomes include:
- Continued seizures and other forms of epilepsy
- Developmental problems
- Autism spectrum disorder
JUMP TO
Disorder Overview
DESCRIPTION
Infantile spasms is a severe form of epilepsy. The term “epilepsy” refers to diseases in which a patient has recurrent seizures. A seizure is an event in which a patient has a change in behavior, such as shaking or loss of awareness. Seizures are caused by abnormal electrical activity in the brain. Infantile spasms is a severe form of epilepsy. In children with infantile spasms, seizures are also called “spasms.”
Infantile spasms is considered severe because of the developmental problems that often occur with the disease.


SIGNS AND SYMPTOMS
The symptoms of infantile spasms can vary.
In some children, infantile spasms will begin without any prior diagnoses or developmental problems. However, in most children, infantile spasms will begin after the diagnosis of another brain disorder. For instance, it can begin after a stroke. Or it can begin after the onset of another form of epilepsy. Some children will already have severe developmental problems when infantile spasms begin.
Typical features of infantile spasms include the following:
Spasm timing
Spasm movements
The movement during a spasm usually includes a quick wide-eyed stare, dropping of the head, and raising of the shoulders and arms. The entire seizure lasts about 1 second. However, there are many possible movements that can happen with a spasm. It is important to note that in an individual child, all of the spasms usually look identical. Examples may be seen here.
Cluster timing
Clusters of spasms may occur once per day. They may occur several times per day. Clusters are most common several minutes after waking. In most cases, there is no warning that spasms are about to happen. However, some parents report that they can predict a cluster is about to happen. They notice a change in their child’s behavior, such as being oddly vigilant or scared. During a cluster of spasms, some children will cry momentarily after each spasm. Others may seem distressed throughout a cluster. Still others will briefly smile or giggle after each spasm. When a cluster is over, children usually go back to their normal behavior.
Developmental problems
Around the time that infantile spasms begin, it is common to observe new developmental problems. These may include a loss of specific “skills.” A child may stop babbling, rolling, sitting, or reaching for objects. Many parents will report that their child seems less alert or engaged. There may be loss of visual fixation and tracking.
Coexisting seizures


CAUSES
There are hundreds of possible causes of infantile spasms. Almost any disease or disorder of the brain can cause it.
Three known types of causes can lead to infantile spasms:
- Abnormalities in the structure of the brain that are present before birth
- Acquired injuries to the brain after birth
- Genetic disorders
The most common causes of infantile spasms include:
- Tuberous sclerosis complex
- Hypoxic-ischemic encephalopathy
- Down syndrome, also called trisomy 21
- Stroke or bleeding in the brain – read more about perinatal stroke and childhood stroke
- Brain malformations such as focal cortical dysplasia, polymicrogyria, hemimegalencephaly, and lissencephaly
- CDKL5 deficiency disorder
- Duplication 15q syndrome, or Dup15q
- Aicardi syndrome
Some children have normal development before infantile spasms, and no cause is found. These children are termed cryptogenic.
TESTING
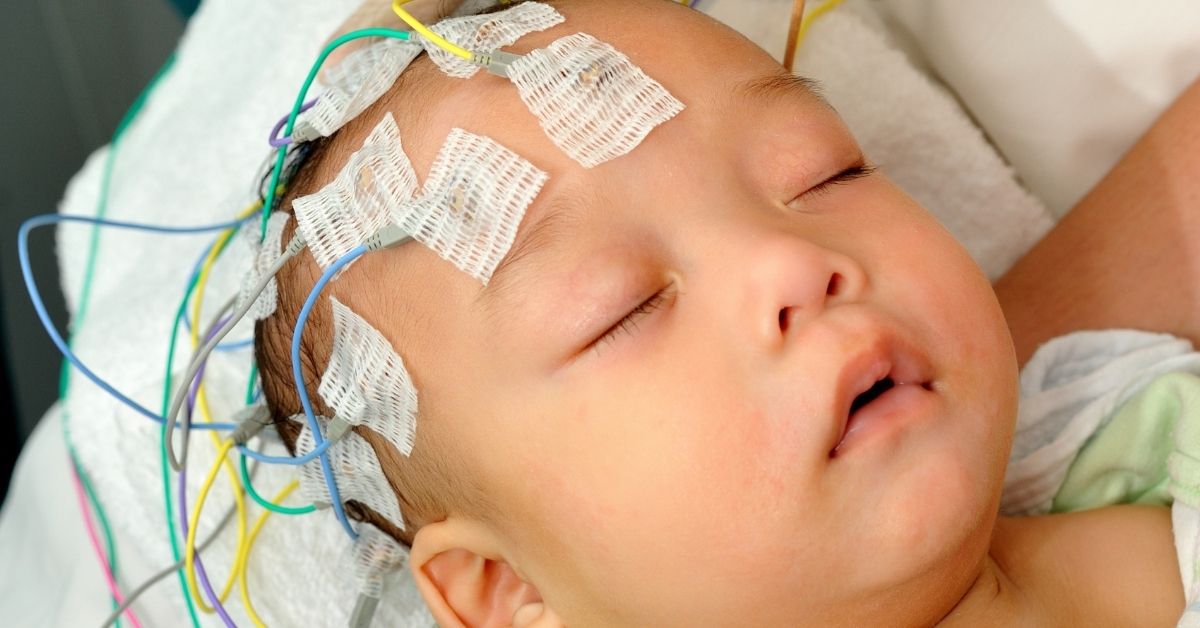
Video-EEG
Infantile spasms is diagnosed with a test called video-electroencephalography (video-EEG). This involves recording video of a child and monitoring their brainwaves. Brainwaves are monitored using about 20 painless electrodes glued to the scalp. A video-EEG test usually lasts between several hours and 24 hours. The first goal of a video-EEG is to see if suspected spasms match with typical electric changes. The second goal is to look for chaotic brainwave abnormalities called hypsarrhythmia. Hypsarrhythmia is sometimes a sign of infantile spasms.
Other Testing
Other testing is often used to search for the cause of infantile spasms.
It may include:
Genetic tests

TREATMENT
There are two first-line treatments for infantile spasms. The first is hormonal therapy. The second is a drug called vigabatrin. These treatments can be used alone or together.
Hormonal Therapy
Hormonal therapy refers to one of two drugs:
- Adrenocorticotropic hormone (ACTH)
- Prednisolone
ACTH and prednisolone are thought to act similarly but there is not strong data to support using prednisolone over ACTH. There is disagreement about which option is best. Treatment protocols vary considerably across hospitals.
There is also some disagreement as to the best dosage and duration of treatment. However, treatment typically requires:
- At least 2 weeks of use at a high dose
- This is followed by a steady reduction in dosage over the following weeks or months
The first treatment leads to resolution of infantile spasms in 40% to 80% of children. About 1 in 3 children who respond to this treatment have a relapse.
Hormonal therapy is generally brief. This is because it can cause many side effects if used for months. There are many possible side effects. However, key risks include:
Immunosuppression


Vigabatrin
Only one traditional anti-seizure medicine has been proven moderately effective at treating infantile spasms. It is called vigabatrin.
It works especially well in some children. These children also have a disorder called tuberous sclerosis complex (TSC). In children without TSC, vigabatrin is somewhat less effective. For those without TSC, response rates are only about 30% to 40%.
About 1 in 3 children who respond to vigabatrin will have a relapse of infantile spasms. This is similar to the relapse rate after hormonal therapy.
The most common side effect of this medicine is fatigue and sedation. However, there are two important but less common vigabatrin side effects. The first is a certain type of vision loss. The second is changes or toxicity in the brain.
Irreversible Peripheral Vision Loss
This results from injury to the retina. The retina is the light-sensing part of the eye. The risk of vision loss is a cause for concern. However, there are several important points to consider:
- Vigabatrin does not lead to complete blindness. In the vast majority of cases, vision loss only occurs at the edges of vision. These edges are known as the periphery. Vigabatrin very rarely seems to affect the important, center part of vision.
- The risk of meaningful vision loss is very low among infants.
- Most important, a child may also lose vision by not treating with vigabatrin. Infantile spasms threaten all brain function. The brain’s role in vision processing can be harmed without successful treatment of infantile spasms. This harm can result in cortical vision impairment, or CVI.
Brain Changes or Toxicity
About 20% of infants who take vigabatrin will have changes in the brain. These changes are not well understood. MRI, or magnetic resonance imaging, is a way of taking pictures of the brain. The changes can be seen with MRI.
The brain changes are almost always reversible. They generally resolve within weeks or months of stopping vigabatrin. The risk of the changes is elevated with higher dosage. It may also be higher among children who take hormonal therapy at the same time. In most cases, the changes are not linked to any symptoms. However, 5% to 10% of infants may have symptoms related to the changes. Specific symptoms depend on which part of the brain is affected.
They can include:
Like changes in the brain MRI, these toxicity symptoms quickly resolve if vigabatrin is stopped. However, the toxicity poses a more significant risk to infants than potential vision loss.


Other Treatments
There are many other treatments for infantile spasms. These treatments are generally less well established. They are also less effective. They include:
- Ketogenic diet
- Pyridoxine
- Topiramate
- Zonisamide
- Felbamate
- Cannabidiol
- Surgical resection, removal of parts of the brain that cause infantile spasms
- Corpus callosotomy, surgical disconnection of the left and right halves of the brain
- Vagus nerve stimulation
OUTLOOK
The long-term outlook for children with infantile spasms varies a lot.
On one hand, most children with infantile spasms do not do well long-term. There are two main reasons for this.
Relapse
Prior disease
On the other hand, normal development and a normal life is possible for some children with infantile spasms. Overall, about 20% of children with infantile spasms will develop normally. A child can develop normally if:
- Infantile spasms is treated quickly and successfully
- A child does not have another severe brain disorder


Resources
Organizations
Infantile Spasms Action Network
The Infantile Spasms Action Network (ISAN) is a collaborative network of over 30 national and international entities focused on raising awareness for infantile spasms. To learn more about the group please visit their website.
Pediatric Epilepsy Surgery Alliance
The Pediatric Epilepsy Surgery Alliance (formerly known as The Brain Recovery Project) enhances the lives of children who need neurosurgery to treat medication-resistant epilepsy. They empower families with research, support services, and impactful programs before, during, and after surgery. PESA’s programs include research-based, reliable information to help parents and caregivers understand when a child’s seizures are drug-resistant; the risks and dangers of seizures; the pros and cons of the various neurosurgeries to treat epilepsy; the medical, cognitive, and behavioral challenges a child may have throughout life; school, financial aid, and life care issues. PESA’s resources include a comprehensive website with downloadable guides, pre-recorded webinars, and virtual workshops; an informative YouTube channel with comprehensive information about epilepsy surgery and its effects; a private Facebook group (Education After Pediatric Epilepsy Surgery) with over 300 members; Power Hour (bi-monthly open forums and live virtual workshops on various topics); and free school training to help your child’s education team understand the impact of their epilepsy surgery in school. Their Peer Support Program will connect you with a parent who has been there. The Pediatric Epilepsy Surgery Alliance also hosts biennial family conferences and regional events that allow families to learn from experts, connect with other families, and form lifelong friendships. They also provide a travel scholarship of up to $1,000 to families in need to fund travel to a level 4 epilepsy center for a surgical evaluation.
In addition, PESA has resources for medical professionals to assist in helping clinicians help the parents of their patients find the resources they need after surgery. Educators and therapists will also find helpful resources and information, including videos, guides, and relevant research. Patients who have undergone surgery are encouraged to register with the Global Pediatric Epilepsy Surgery Registry to help set future research priorities.


Publications
JCN Podcast on Infantile Spasms: An interview with Dr. Rana Said
Podcast from SAGE Neuroscience and Neurology/Journal of Child Neurology (JCN). Dr. Angela Curcio of Columbia University Medical Center and a member of JCN and CNO’s Residents & Fellows Board interviews Dr. Rana Said of UT Southwestern Medical Center on her research on infantile spasms and career in pediatric neurology.
JCN: NICU Series- Interview with a Parent and the Brain Recovery Project: Childhood Epilepsy Foundation
Podcast from SAGE Neuroscience and Neurology/Journal of Child Neurology (JCN). Dr. Sonika Agarwal of Children’s Hospital of Philadelphia talks to Audrey Vernick about her experience with pediatric epilepsy, perinatal stroke, and infantile spasms from a parent’s perspective. Brain Recovery Project website.
Child Neurology Foundation (CNF) solicits resources from the community to be included on this webpage through an application process. CNF reserves the right to remove entities at any time if information is deemed inappropriate or inconsistent with the mission, vision, and values of CNF.
Research
ClincalTrials.gov for Infantile Spasms are clinical trials that are recruiting or will be recruiting. Updates are made daily, so you are encouraged to check back frequently.
ClinicalTrials.gov is a database of privately and publicly funded clinical studies conducted around the world. This is a resource provided by the U.S. National Library of Medicine (NLM), which is an institute within the National Institutes of Health (NIH). Listing a study does not mean it has been evaluated by the U.S. Federal Government. Please read the NLM disclaimer for details.
Before participating in a study, you are encouraged to talk to your health care provider and learn about the risks and potential benefits.
The information in the CNF Child Neurology Disorder Directory is not intended to provide diagnosis, treatment, or medical advice and should not be considered a substitute for advice from a healthcare professional. Content provided is for informational purposes only. CNF is not responsible for actions taken based on the information included on this webpage. Please consult with a physician or other healthcare professional regarding any medical or health related diagnosis or treatment options.
References
“Signs of infantile spasms” [Video]
https://www.youtube.com/watch?v=kRt8muFfUQo&t=19s
“Infantile spasms: Know the signs and take action” [Video]
https://www.youtube.com/watch?v=6nOKqTxYJFU
“Treatment of infantile spasms” [Open Access Scientific article]
https://onlinelibrary.wiley.com/doi/full/10.1002/epi4.12264
“West syndrome: A comprehensive review” [Open Access Scientific article]
https://link.springer.com/content/pdf/10.1007/s10072-020-04600-5.pdf
Thank you to our 2023 Disorder Directory partners:





