

Rylae-Ann as a baby
Richard Poullin and Judy Wei live in Thailand with their 4-year-old daughter Rylae-Ann.
Although Judy says her pregnancy and delivery were uncomplicated, when Rylae-Ann was 3 months old they noticed their baby seemed lethargic, restless, and sometimes very unhappy.
“She wasn’t meeting her developmental milestones,” Judy said. “She couldn’t sit, turn, move or grab. She was responsive in her eyes and would be happy to see us, but most of the time, she was crying or sleepy.”
The days and nights became long and worrisome, as Richard and Judy noticed that Rylae-Ann couldn’t even breathe comfortably because her neck muscles were so weak. They would have to take turns carrying her round-the-clock so that she could be supported and comfortable.
This was the beginning of their diagnostic odyssey. They would take Rylae-Ann to the hospital, and over and over, the doctors told them it was epilepsy. So Richard and Judy did everything they could to learn about epilepsy, including connecting with the CNF’s Family Support Program.
Doctors put her on a seizure medication, but based on what Richard and Judy knew about seizures and what they saw at home with their daughter – both her initial symptoms and the horrible side effects from the medication – they knew in their gut this wasn’t the correct route.
Rylae-Ann’s ‘spells’ (what the doctors mistook for seizures) had unique traits. Her eyes would cross and go up, and her tongue would thrust out. Her body would start twisting, and then finally – sometimes after eight or more hours – her spell would end, and she would fall asleep. And most notable was that these spells would happen every three days.
Because they happened in a predictable pattern, Judy and Richard decided to take Rylae-Ann to the hospital before they knew one was coming so that the doctors could monitor her and see it in real-time. At this point, the doctors agreed that it wasn’t epilepsy but instead diagnosed her with dystonia and gave her another medication.
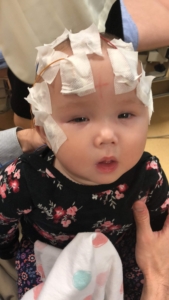

Rylae-Ann during an EEG
“In hindsight, we don’t fault any of the doctors,” Judy and Richard said. “ We would find out later that Rylae-Ann has a rare disease that not many people know about. But at this point, when we were stuck on this journey of trying to figure things out, we just kept trusting our gut. What we heard wasn’t sitting right with us.”
Around this time, when Rylae-Ann was 8 months old, they first heard about AADC Deficiency. Judy’s brother sent her a link to a story about a child with AADC who had almost identical symptoms as Rylae-Ann. This led Richard and Judy to find a doctor in Taiwan who is familiar with this condition and runs a gene therapy clinical trial. Thanks to a bout of good luck, they scheduled an appointment within a week of learning about him.
“We flew to Taiwan on Christmas Eve to meet this doctor,” Judy said. “He asked questions, examined her, and after carrying her for just five minutes, he was able to say, ‘Yes, I think this is AADC Deficiency. Let’s run some tests to be sure.’”
By now, the family had spent five months searching for a diagnosis, which is very short compared to most of the rare disease community.
“It just shows that the diagnostic process, when someone knows what conditions to look for, it doesn’t have to be invasive or painful, and it could be quick,” said Richard. “If we had seen him when she was much younger, it would have saved a lot of grief.”
Now armed with an official and accurate diagnosis of AADC, Richard and Judy wanted to enroll Rylae-Ann in the clinical trial that the doctor in Taiwan was running. After checking all the boxes to make sure she was eligible – obtaining a Taiwanese passport and running more tests – they had to wait another year until she was old enough for the actual surgery that the therapy consisted of.
During that year of waiting, although it was devastating and isolating, Richard and Judy held on to hope that they were at least making progress and doing more of the ‘right’ things to help their daughter.
“Now that we knew that she wasn’t having seizures and that her spells were actually something called oculogyric crises (OGC), we could be more confident in what to do with her,” Judy said. “Before, we were afraid to ‘push’ her or move her too much because we thought it would trigger a seizure. But since her spells are OGCs, we know that those will happen no matter what, so we were able to work with her on movement and mobility.”
This is another way a diagnosis changed their perspective. Every bit of work and therapy they did with Rylae-Ann before the gene therapy surgery would only help her pick up on movement and mobility more quickly afterward.
“The hardest part is that we felt so alone,” they said. “We had no one to go to, and there was such limited information about AADC. We had no idea what to expect and did not have much help. But we tried hard to be the care team she needed, and we made things work.”
Richard and Judy said that online resources like the ones that CNF offered were so helpful during this isolating year. They would find resources and information that overlapped with what they were experiencing, even if it wasn’t the same diagnosis, and they could adapt them to their situation.
“The best things were the patient stories,” Richard said. “They helped us feel less alone, and although it would take some time, they inspired us to start being more open to sharing our stories in the hope that we could help another family.
“The family stories on CNF’s website gave us hope, so we want to be that voice for others.”
In the spirit of sharing their story to help others, Richard and Judy worked with Dr. Heather Mefford to help her develop some of CNF’s Shortening the Diagnostic Odyssey resources.
They also continue to use CNF’s content as inspiration. They adapt what they can for Rylae-Ann, and share things with families they work with through their new nonprofit, TeachRare, which helps caregivers embrace a therapy- and education-based lifestyle change when their child is diagnosed with a rare disease.


Rylae-Ann playing at school

